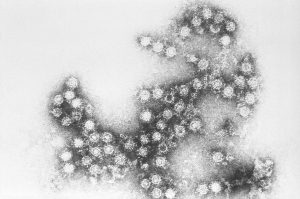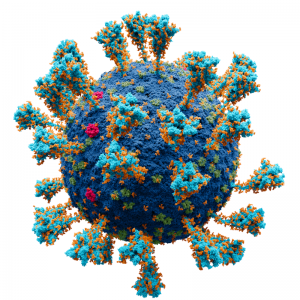
Coronavirus
including covid-19
COVID-19 transmits when people breathe in air contaminated by droplets and small airborne particles containing the virus. The risk of breathing these in is highest indoors. Transmission can also occur if splashed or sprayed with contaminated fluids in the eyes, nose or mouth and via contaminated surfaces.
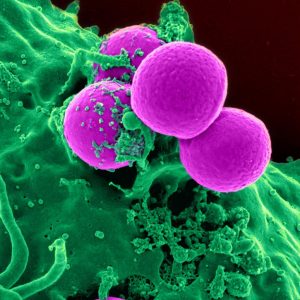
mrsa
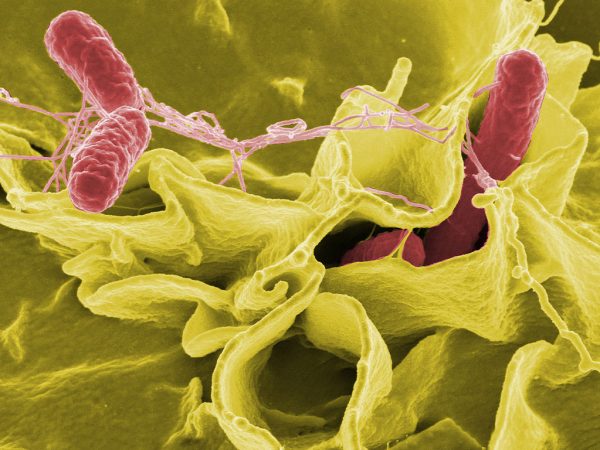
Salmonella
food poisoning
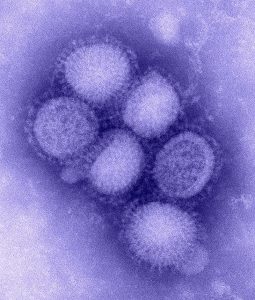
Influenza
H1N1 SWINE FLU and H5N1 bird flu
Well known outbreaks of H1N1 strains in humans include the 2009 swine flu pandemic, the 1977 Russian flu pandemic as well as the 1918 flu pandemic. It is an orthomyxovirus that contains the glycoproteins haemagglutinin and neuraminidase. For this reason, they are described as H1N1, H1N2 etc. depending on the type of H or N antigens they express with metabolic synergy. Some strains of H1N1 are endemic in humans and cause a small fraction of all influenza-like illness and a small fraction of all seasonal influenza, for instance in 2004–2005. Other strains of H1N1 are endemic in pigs (swine influenza) and in birds (avian influenza).
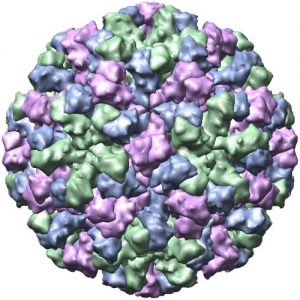
Norovirus
the most common cause of gastroenteritis